Diabetes Doctor
Are You Tired Of Dealing With Pricks?
Our Diabetes Doctor Provides a Complete Plan To Manage Diabetes And A Healthy Lifestyle
See Our Diabetes Doctor For Effective Treatment
Diabetes mellitus is a disorder in which the body does not produce enough or normally respond to insulin, causing blood sugar (glucose) levels to be abnormally high. Urination and thirst increase and people may lose weight even if they are not trying. Visit UrgentWay if you are witnessing any of these symptoms.
Diabetes includes type 1 diabetes and type 2 diabetes. Conditions for potentially reversible diabetes include prediabetes and gestational diabetes. Prediabetes occurs when your blood sugar is higher than usual but not high enough to qualify as diabetes. Prediabetes is often a precursor to diabetes unless appropriate measures are taken to prevent progression. Gestational diabetes occurs during pregnancy but can disappear after childbirth.
The cause of diabetes varies from type to type. But no matter what kind of diabetes you have, it can lead to excessive blood sugar, which may cause serious health issues.
Our board certified providers will discuss your health and counsel you on preventative care and healthy choices.
Book Your
Appointment Now
Superior Health Care
Pay $0 With Insurance
Rated 5 Stars
Superior Health Care
Pay $0 With Insurance
Rated 5 Stars
- Certified providers
- In and out in 30 minutes
- No referral required
- 500,000+ Satisfied patients
- OPEN EVERY DAY OF THE YEAR
- Full-service After Care
- Gold Seal of Approval
- Who's Who Award Winner
URGENTWAY
Providing Accessible premium care without the wait
URGENTWAY
Providing Accessible Premium Care Without The Wait


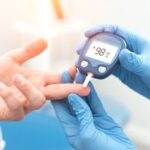





Care That's Convenient and Affordable

Affordable
You can get your diagnosis and treatment at a low cost at any of our locations. No hidden charges.

Certified Physicians
Our certified physicians, including Diabetes Doctors, provide a thorough diagnosis and treatment.
When Do You Need To See a Diabetes Doctor?
Treatment for type 1 diabetes includes insulin injections or the use of an insulin pump, frequent blood sugar tracking, and carbohydrate counting. Treatment for type 2 diabetes primarily includes lifestyle changes, blood sugar control, and medications for diabetes, insulin, or both.
Healthy lifestyle choices can help you bring your blood sugar back to normal or at least prevent it from rising to the levels seen in type 2 diabetes. Maintaining a healthy weight through exercise and a healthy diet can help.
Qualified to Heal You
Who's Who Top Doctors In America Award Winner
We are Certified & Accredited
We are Certified & Accredited


We are Certified & Accredited




UrgentWay Achievements
1
M+PATIENTS SEEN
10
K+POSITIVE REVIEWS
2
M+LAB TESTS
250
K+VACCINATIONS
350
K+COVID TESTS

UrgentWay Telemedicine Service
Book your online session with our health care professional and get yourself treated from the comfort of your own home.
UrgentWay Telemedicine Service
Book your online session with our health care professional and get yourself treated from the comfort of your own home.

We Are Valued By Our Community

Great experience at this urgent care! Quick and efficient! The staff is very friendly and courteous and the level of care is extremely exceptional.
The front desk girl Adarsh is very quick and knowledgeable. She had me in to see the medical assistant within minutes who made me feel very comfortable.
The Provider helped me with all my needs.
Amazing service, def recommend!!

Monisha Lal
PatientAmazing Service!!! I have been here twice for my Covid test due to traveling and front desk is THE BEST ! As a receptionist myself I know good service and bad when I see it and these girls hold it down with those phone calls while giving great costumer service upfront in office . Thank You Toby, Vanessa and Enais !! Nurses where fantastic and test went smooth.

ERIKA M
PatientDefinitely will be returning to this facility, walked into the door to a bright and welcoming face. The front desk girl very quickly registered me, and i was taken back for my vitals. Provider was also very attentive to my concerns. Very quick efficient services with great friendly staff. Came to this office as it was nearby my work.. was in and out of the office in 45 minutes. Really recommend this place!

amir pal
PatientOur Diabetes Doctors Are Known For Providing the Best Counseling At UrgentWay Regarding Diabetes:
Our healthcare providers advise checking your feet for early diagnosis of diabetes. Inspect your feet every day, especially between the toes and the sole, for cuts, bruises, cracks, blisters, redness, ulcers, and any sign of abnormality. Each time you visit a health care provider, remove your shoes and socks so your feet can be examined. Any problems that are discovered should be reported to your Diabetes Doctor or a medical professional as soon as possible, no matter how “simple” it may seem to you.
The key to successful wound healing is regular medical care from your Diabetes Doctor to ensure the following “gold standard” of care:
- Lowering blood sugar
- Appropriate debridement of wounds
- Treating any infection
- Reducing friction and pressure
- Restoring adequate blood flow
Our Diabetes Doctors Provide The Best Diabetes Treatment And Management Plans At UrgentWay Clinics
The cause of diabetes varies from type to type. But no matter what type of diabetes you have, it can lead to excessive blood sugar which can lead to serious health problems. Our board-certified providers can tailor treatment according to your need for a healthy life style.
UrgentWay Support
We are here to listen to your positive feedback, answer your queries, and provide support. If you have a question or you want to book, cancel, reschedule your appointment, or need your results, then just give us a call. We are only a call away.
UrgentWay Support
Call : (551) 325-3250
UrgentWay Support
We are here to listen to your positive feedback, answer your queries, and provide support. If you have a question or you want to book, cancel, reschedule your appointment, or need your results, then just give us a call. We are only a call away.
UrgentWay Support
Call : (551) 325-3250
We accept all major insurances
Medicare Plans, Aetna, Cigna, Oscar, United Healthcare, Emblem Health, Health Net, Magnacare…
Illness & Injuries
Primary Care
Pediatrics Care
School Physicals
Vaccination

Lab Tests
Employee Physicals
STD Screening
Immigration
DOT/TLC Exams
Frequently Asked Questions

What Is A Diabetic Foot Ulcer?
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes and is commonly located on the bottom of the foot.
Diabetic Patients who develop a foot ulcer, six percent will be hospitalized due to infection or other ulcer-related complications.
Diabetes is the leading cause of nontraumatic lower extremity amputations in the United States, and approximately 14 to 24 percent of patients with diabetes who develop a foot ulcer have an amputation. Research has shown that the development of a foot ulcer is preventable.
Who Can Get A Diabetic Foot Ulcer?
Anyone who has diabetes can develop a foot ulcer. Native Americans, African Americans, Hispanics, and older men are more likely to develop ulcers. People who use insulin are at a higher risk of developing a foot ulcer, as are patients with diabetes-related kidney, eye, and heart disease. Being overweight and using alcohol and tobacco also play a role in the development of foot ulcers. Consult our healthcare providers for more information.
How Do Diabetic Foot Ulcers Form?
Ulcers form due to a combination of factors, such as lack of feeling in the foot, poor circulation, foot deformities, irritation (such as friction or pressure), and trauma, as well as the duration of diabetes.
Patients who have had diabetes for many years can develop neuropathy, a reduced or complete lack of ability to feel pain in the feet due to nerve damage caused by elevated blood glucose levels. Nerve damage can often occur without pain, and one may not even be aware of the problem. Vascular disease can complicate a foot ulcer, reducing the body’s ability to heal and increasing the risk of infection. Elevations in blood glucose can reduce the body’s ability to fight off a potential infection and also retard healing. Early detection and care are important; book your appointment today with UrgentWay’s certified healthcare provider.
What Is The Risk Of Not Treating A Diabetic Foot Ulcer?
Once an ulcer is noticed, contact the urgentway medical center immediately for prompt medical care. Foot ulcers in patients with diabetes should be treated for several reasons:
- To reduce the risk of infection and amputation
- To improve function and quality of life
- To reduce health care costs
How Should A Diabetic Foot Ulcer Be Treated?
The primary goal in the treatment of foot ulcers is to heal the wound as soon as possible and reduce the risk of infection.
There are. several key factors in the appropriate treatment of a diabetic foot ulcer:
- Taking the pressure off the area, called “off-loading”
- Removing dead skin and tissue, called “debridement”
- Applying medication or dressings to the ulcer
- Managing blood glucose and other health problems
How Can A Foot Ulcer Be Prevented?
The best way to treat a diabetic foot ulcer is to prevent its development in the first place. Recommended guidelines include seeing your Doctor/healthcare provider regularly. Your Doctor/healthcare provider can determine if you are at high risk for developing a foot ulcer and together implement strategies for prevention.
You are at high risk:
- Have neuropathy
- Have poor circulation
- Have a foot deformity (i.e. bunion, hammer toe)
- Wear inappropriate shoes
- Have uncontrolled blood sugar
The signs and symptoms of type 1 diabetes and type 2 diabetes
The Signs And Symptoms Of Type 1 Diabetes And Type 2 Diabetes Are:
- Dehydration – increased thirst
- Extreme hunger
- Unexplained gradual weight loss
- Increased urination frequency
- Fatigue
- Irritability
- Blurry vision
- Slow-healing sores
- Recurrent frequent gum, skin, and vaginal infection
What Can I Eat If I Have Diabetes?
You can eat just about anything you want. It is about knowing proper meal portions and how much you are putting on your plate. A Diabetes helathcare provider can help you learn to count carbohydrates and develop a meal plan that is specific for you.
Some Simple Ways To Reduce The Risk Of Getting Diabetes:
- Reduce your total carbohydrate intake
- Exercise regularly
- Maintain water intake
- Try to lose extra weight
- Give up smoking
- Reduce meal portion
- Reduce sedentary lifestyle
- Follow a high-fiber diet
- Optimize vitamin D levels
- Reduce your consumption of processed foods
What Foods Have Carbohydrates?
The following foods have carbohydrates:
- Fruits, starchy vegetables, milk, yogurt, rice, cereals, bread, and other grains.
- Snack foods, such as pretzels, chips, and popcorn, have carbs.
- Sweets, regular soda, cakes, candy, and cookies, also contain carbohydrates.
What Are Some Common Factors That Increase The Risk Of Getting Diabetes?
- Overweight
- Family history
- Race or ethnicity
- Diabetes during pregnancy
- Polycystic ovary syndrome
- High blood pressure
- Abnormal levels of cholesterol and triglycerides
What Should My Blood Sugar Be?
The American Diabetes Association recommends a blood glucose range of
- 80-130 before meals
- less than 180 about 2 hours after a meal.
What Is An A1c?
Hemoglobin A1c is a 2-3 month average of your blood sugars. This result gives you a good idea of how well your diabetes is being managed/controlled. The American Diabetes Association recommends an A1c of less than 7 to keep the risk of complications low. Consult our health care providers to learn about the complications of higher A1C levels.
Do I Need To Follow A Low-Carb Diet?
Carbohydrates are an important part of a healthy diet. Diabetic patients are recommended to watch portion sizes and are advised to get the most of their carbs from fruits, vegetables, whole grains, and low-fat milk and yogurt. Diabetic patients can also benefit from eating lower-fat, high-fiber foods and consume enough calories to maintain a healthy weight.
If It Is Sugar-Free, I Can Eat As Much As I Want, Right?
Sugar-free foods can be part of a healthy meal plan in small amounts. Keep in mind that some of these foods still have carbs (in the form of other sweeteners such as sorbitol, isomalt, and mannitol) and may affect your blood glucose levels. Many sugar-free foods have calories and carbohydrates, and lots of fat. Make sure you read the nutrition labels.
- (646) 213-0190
- Mon – Fri: 9:00 AM to 6:00 PM
- Sat – Sun: Closed
- (347) 934-9045
- Mon – Fri: 9:00 AM to 7:00 PM
- Sat – Sun: 9:00 AM to 4:00 PM
- (516) 489-6600
- Mon – Fri: 9:00 AM to 8:00 PM
- Sat – Sun: 9:00 AM to 4:00 PM
- (516) 252-3903
- Mon – Fri: 9:00 AM to 8:00 PM
- Sat – Sun: 9:00 AM to 4:00 PM
Urgent Care
UrgentWay is dedicated to provide you with the right care when you need it the most. Just give us a call and talk to the best health care professionals.
Primary Care
Our Primary Care services focus on preventative medicine and regular follow-ups to develop a long-term trustworthy relationships with patients.
Urgent Care
UrgentWay is dedicated to providing you with the right care when you need it most. Just give us a call and talk to the best health care professionals.
Primary Care
Our Primary Care services focus on preventative medicine and regular follow-ups to develop a long-term trusting relationship with patients.

